If sex has become painful, your desire has dropped, or you feel drier and less sensitive than you used to, you are not alone and you are not imagining it. Millions of women experience sexual dysfunction at some point in their lives, especially after hormonal shifts from childbirth, perimenopause, or menopause. And for a long time, the treatment options were limited: hormonal creams, lubricants, or surgery.
But there is a newer option that has been gaining serious attention in gynecology and sexual medicine: PRP injections (platelet-rich plasma therapy) applied directly to the vaginal and clitoral area to restore sensitivity, lubrication, and sexual function from the inside out.
This article explains exactly what PRP injections do for women’s sexual health, who they are designed for, what the clinical research actually shows, and what to look for when choosing a provider.
Important: This article covers two related conditions: female sexual dysfunction (FSD) and stress urinary incontinence (SUI), because they often affect the same women and are treated with PRP using similar approaches. You will find clear, separate sections for each.
Scientific Source: This article is based on peer-reviewed research by I. Dankova, N. Pyrgidis, M. Tishukov, E. Georgiadou, M.P. Nigdelis, E.-F. Solomayer, J. Marcon, C.G. Stief, and D. Hatzichristou, “Efficacy and Safety of Platelet-Rich Plasma Injections for the Treatment of Female Sexual Dysfunction and Stress Urinary Incontinence: A Systematic Review,” published in Biomedicines, 2023, Vol. 11, 2919. DOI: https://doi.org/10.3390/biomedicines11112919
Key Takeaways: (TL;DR)
- PRP injections for female sexual dysfunction involve injecting a concentrate made from your own blood into the vaginal wall and clitoris to stimulate tissue regeneration.
- Clinical studies report significant improvements in sexual desire, arousal, lubrication, orgasm, and vaginal health scores after PRP treatment.
- PRP also shows measurable results for stress urinary incontinence (urine leakage during coughing or exercise), though surgery still outperforms it in that area.
- The standard protocol is 3 monthly sessions; serious side effects were rare (less than 1%).
- PRP is not yet in official clinical guidelines (it is investigational) but results so far are promising enough that specialists are using it in clinical settings.
So What Is PRP and Why Are Doctors Injecting It Into the Vaginal Area?
PRP stands for platelet-rich plasma. It is a concentrated solution made from your own blood that contains a high density of platelets, the cells your body uses to heal tissue, grow new blood vessels, protect nerves, and regulate inflammation.
When PRP is injected into the vaginal wall or clitoris, the theory is that those growth factors stimulate the local tissue to regenerate: forming new blood vessels, increasing collagen, improving nerve sensitivity, and restoring the health of the vaginal lining.
This is the same regenerative principle used in orthopedic medicine, wound care, and dental surgery, applied to female pelvic and sexual health.
Other Names You Might See for This Treatment
O-Shot (Orgasm Shot)
The most widely recognized brand name for vaginal and clitoral PRP injections, used specifically for sexual enhancement and dysfunction
Autologous platelet-rich plasma (A-PRP)
A medical term emphasizing the plasma comes from your own body
PRP vaginal rejuvenation
A term used in cosmetic and aesthetic medicine
Platelet-rich fibrin matrix
A variation where the PRP is mixed with calcium chloride to form a gel-like substance before injection
Preparation kits used by clinics in the studies include RegenKit® and TruPRP®. Some providers also add hyaluronic acid to the mixture, which may enhance the moisturizing and volumizing effect in the vaginal tissue.
What Do All These Abbreviations Actually Mean?
| Abbreviation | Full Name | Measures | Score Range | Better Score |
| FSFI | Female Sexual Function Index | Overall sexual function (desire, arousal, lubrication, orgasm, satisfaction, pain) | 1 to 36 | Higher (below 26.55 = dysfunction) |
| FSDS-R | Female Sexual Distress Scale Revised | Emotional distress related to sexual activity | 0 to 48 | Lower (15+ = distress) |
| VHI | Vaginal Health Index | Vaginal moisture, elasticity, secretions, pH, epithelial integrity | 5 to 25 | Higher (below 15 = atrophy) |
| FGSIS | Female Genital Self-Image Scale | A woman’s feelings about her own genitals and sexual body image | 7 to 28 | Higher |
| ICIQ-SF | International Consultation on Incontinence Questionnaire Short Form | Severity of urinary incontinence | 0 to 21 | Lower |
| UDI-6 | Urogenital Distress Inventory-6 | Disability and quality of life impact from urinary symptoms | 0 to 100 | Lower |
What Exactly Happens During a PRP Session for Sexual Dysfunction?
The procedure does not involve surgery, incisions, or general anesthesia. Here is how it works from start to finish:
- Blood draw: A small blood sample is taken from your arm, just like a routine blood test.
- Processing: The blood is mixed with an anticoagulant to prevent clotting, then placed into a centrifuge machine that spins it at high speed for several minutes.
- Separation: The centrifuge separates the blood into layers. The platelet-rich plasma, now containing 1.6 to 6 times more platelets than normal blood, is extracted.
- Optional activation: Some protocols add calcium chloride to activate the platelets and transform the PRP into a fibrin matrix before injection.
- Injection: The concentrated PRP is injected into the targeted area using a fine needle. For sexual dysfunction, this is typically the distal anterior vaginal wall and sometimes the clitoris.
Where Is the Injection Given and Why That Specific Spot?
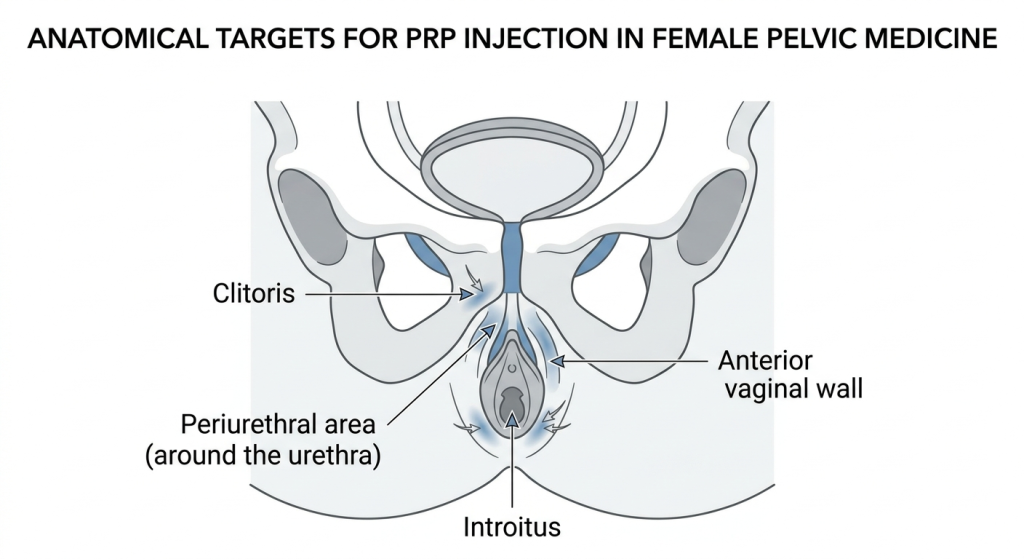
For female sexual dysfunction, the distal anterior vaginal wall is the preferred injection site. Research shows this region has a significantly higher density of nerves and blood vessels compared to other parts of the vaginal wall, which means PRP injected there can have the greatest regenerative impact on sexual sensitivity and tissue health.
Some studies also injected PRP directly into the clitoris and the introitus (vaginal opening) area.
| Condition Being Treated | Where PRP Is Injected | How Much (per session) | How Often |
| Female Sexual Dysfunction (FSD) | Anterior vaginal wall, clitoris, introitus | 2 mL | Once a month, 3 sessions total |
| Stress Urinary Incontinence (SUI) | Periurethral area (around the urethra) | 5 to 6 mL | Once a month, 3 sessions total |
Which Women Is This Treatment Actually Designed For?
PRP injections for sexual health are not a one-size-fits-all solution. Based on the clinical studies reviewed, here is who may benefit most:
Women with Female Sexual Dysfunction (FSD)
FSD is an umbrella term that covers several problems affecting a woman’s sexual experience:
- Low sexual desire or interest (hypoactive sexual desire disorder)
- Difficulty with arousal, not feeling physically or mentally engaged during sex
- Difficulty reaching orgasm or reduced orgasm intensity
- Pain during sex (dyspareunia), which often comes from vaginal dryness and thinning caused by estrogen loss
- Vulvovaginal atrophy, a condition common after menopause where the vaginal walls become thinner, drier, and less elastic
The women included in FSD studies had a mean age of around 49 years. Many were postmenopausal. PRP may be a particularly useful option for women who:
- Want to avoid or cannot use hormonal therapy
- Have tried lubricants and moisturizers with limited results
- Experience sexual distress (anxiety, frustration, or emotional difficulty related to sexual problems)
- Have vulvovaginal atrophy that is affecting their intimate life and well-being
Women with Stress Urinary Incontinence (SUI)
SUI means leaking urine during physical activities that put pressure on the abdomen, like coughing, sneezing, laughing, jumping, or exercising. It is separate from urgency incontinence (the sudden urge to urinate).
Women in SUI studies had a mean age of around 53 years. PRP for SUI may suit women who:
- Want a non-surgical approach before committing to an operation
- Have tried pelvic floor physiotherapy without sufficient improvement
- Are not suitable candidates for surgery due to health or personal reasons
Worth knowing: The only randomized controlled trial in this review compared PRP directly to a midurethral sling (the standard surgical fix for SUI) and found the surgery produced better scores. PRP for SUI is not a replacement for surgery, it is an alternative for women who prefer to avoid it.
The Real Results: What Clinical Studies Found for Female Sexual Dysfunction
Five studies covering 172 women with female sexual dysfunction all received PRP therapy and were tracked using validated clinical tools. Here is what was measured and what changed:
Sexual Function Scores (FSFI)
The Female Sexual Function Index (FSFI) is the gold standard tool for measuring overall sexual function in women. It scores arousal, lubrication, orgasm, satisfaction, desire, and pain on a scale from 1 to 36. A score below 26.55 indicates dysfunction.
| Study | FSFI Before PRP | FSFI After PRP | Change | Statistically Significant? |
| Sukgen et al. | 14.0 | 28.0 | +14 points | Yes (p < 0.001) |
| Runels et al. | 24.0 | 30.0 | +5.5 points (mean) | Yes (p = 0.01) |
A jump from 14 to 28 on the FSFI is substantial, it represents the difference between significant sexual dysfunction and scores within the normal range. Both studies showed statistically significant improvement.
Vaginal Health and Atrophy Scores (VHI)
The Vaginal Health Index (VHI) measures moisture, secretions, elasticity, pH, and the overall health of the vaginal lining. A score below 15 indicates vulvovaginal atrophy. After PRP:
| Study | VHI Before PRP | VHI After PRP | Statistically Significant? |
| Hersant et al. | 11.0 | 21.0 | Yes (p < 0.001) |
| Saleh et al. | 12.0 | 17.0 | Yes (p < 0.001) |
Both studies showed VHI scores moving from the atrophy range into healthy territory. Women reported less dryness, less discomfort, and better lubrication after PRP sessions.
Sexual Distress Scores (FSDS)
The Female Sexual Distress Scale measures the emotional burden of sexual dysfunction; feelings like frustration, worry, and anxiety about one’s sex life. Lower scores mean less distress.
After PRP, Hersant et al. reported a drop in FSDS from 36.0 to 30.0 (p < 0.001). Runels et al. reported a drop from 17 to 7.3, a more than 50% reduction in sexual distress.
Self-Image and Self-Esteem
One study (Sukgen et al.) also tracked genital self-image using the Female Genital Self-Image Scale (FGSIS) and found significant improvement (from 17 to 24) suggesting that beyond physical symptoms, PRP may also help restore a woman’s confidence in her own body.
Results for Urinary Leakage: What the Numbers Show
Seven studies involving 155 women with stress urinary incontinence evaluated PRP therapy. Across all seven, incontinence symptoms improved after treatment.
| Measurement | Before PRP | After PRP | Significant? |
| ICIQ-SF (incontinence severity, 0-21) | 12.0 to 18.0 | 5.0 to 8.0 | Yes (p < 0.01) |
| UDI-6 (quality of life disability, 0-100) | 35.0 to 39.0 | 6.6 to 28.0 | Yes (p < 0.01) |
| 1-Hour Pad Test (urine leaked) | 15 grams | 6.2 grams | Yes (p < 0.001) |
| Cough Stress Test (leakage on coughing) | 100% positive | 30% positive | Yes |
Is It Safe? Here Is Every Side Effect Reported Across All 317 Women
Across all 12 included studies, only 3 out of 317 women who received PRP injections experienced any side effects at all and none of those were serious. Specifically:
- 2 women treated for sexual dysfunction experienced heightened sexual arousal after treatment (including continuous arousal and spontaneous orgasm). This resolved on its own without any intervention.
- 1 woman treated for urinary incontinence developed temporary urinary retention that required self-catheterization for a few days. This also resolved without further treatment.
No infections, no bleeding, no nerve damage, and no serious adverse events were reported in any of the studies. This safety profile is consistent with how PRP performs in other medical fields such as orthopedics, dental surgery, and wound care.
How Often Do You Actually Need PRP Injections?
Based on the protocols used across all 12 studies, here is what most providers follow:
- 3 sessions total, with one session per month for three consecutive months
- For sexual dysfunction: 2 mL per session into the anterior vaginal wall (and sometimes clitoris)
- For urinary incontinence: 5 to 6 mL per session into the periurethral area
Some patients in the studies received fewer sessions (as few as one) and some received up to five sessions over four months, depending on individual response.
The studies did not find one universally agreed-upon number of sessions, this is one of the areas the review identified as needing more research.
After the initial course, follow-up was tracked for up to 12 months. There is currently no published data on what happens after 12 months; whether results fade, remain stable, or require a maintenance session.
How to Choose the Right Clinic or Doctor for This Procedure
Not all PRP is created equal and not all providers have the training needed to do this properly. Here is what to look for before booking:
They Use a Validated PRP Preparation Kit
Ask the clinic which preparation system they use. The studies in this review used validated commercial kits such as RegenKit® and TruPRP®. A provider who uses an unverified or improvised system cannot guarantee the platelet concentration or quality of the PRP being injected.
They Assess You with Recognized Clinical Tools
A quality provider will use validated questionnaires to assess your symptoms before treatment starts and at each follow-up. For sexual dysfunction, the FSFI and FSDS-R are the standard tools. For urinary leakage, it is the ICIQ-SF and UDI-6.
If your clinic is not measuring your baseline and tracking your progress with these tools, they cannot tell you objectively whether the treatment is working.
The Doctor Has Specialist Training in Female Pelvic Health
PRP injections for women’s sexual health belong in the hands of gynecologists, urogynecologists, or specialists in female pelvic medicine, not general aesthetic clinics or providers who have added this as an upsell.
Ask directly about the provider’s specialty and their experience with this specific procedure.
They Are Honest About the Limitations
A trustworthy provider will tell you upfront that PRP for sexual dysfunction is still investigational. It is not a guaranteed cure. No ethical specialist should promise specific results or use pressure tactics. If the clinic sounds more like a sales pitch than a medical consultation, look elsewhere.
They Have a Structured Follow-Up Plan
Research follow-up in the studies was tracked for up to 12 months. Your provider should reassess you at 3 months and again at 6 to 12 months after your last session to measure your progress. A clinic that does not offer post-treatment monitoring is not following the standards of care reflected in the clinical research.

Women’s Sexual Wellness
Myths vs. Reality: What Women Are Often Told (and What the Research Actually Says)
| What You Might Have Heard | What the Research Actually Shows |
| “PRP will permanently fix your sexual dysfunction.” | Studies tracked patients for up to 12 months. No data exists beyond that on how long the effects last. |
| “One injection is enough to see results.” | The standard protocol across most studies was 3 injections over 3 months, not a single session. |
| “Any doctor can do this procedure.” | Proper PRP preparation requires validated kits, centrifugation, and specialist knowledge of pelvic anatomy. |
| “PRP is an approved standard treatment.” | It is not in official clinical guidelines yet and is still classified as investigational. |
| “The results are the same regardless of how the PRP is prepared.” | Platelet concentration, preparation technique, and injection volume all vary significantly between providers and affect outcomes. |
| “PRP will cure urinary leakage completely.” | Most women improved significantly, but the only randomized trial showed surgery still outperformed PRP for SUI at 3 months. |
Summary
PRP injections for female sexual dysfunction represent one of the most genuinely interesting advances in women’s intimate health in recent years. The science behind it is logical, using your body’s own healing mechanisms to restore tissue quality, sensitivity, and function in an area that is central to quality of life.
The clinical research reviewed here shows real, statistically significant improvements in sexual function, vaginal health, and sexual distress in women who received PRP treatment.
Side effects were minimal and resolved on their own. For women with urinary leakage, results were also meaningful, though surgery remains more effective for that condition.
The honest caveat is that this is still emerging medicine. Studies have been small. No one has tracked patients beyond 12 months. And the treatment is not yet in official guidelines. But the signal is positive enough that specialists are using it in clinical settings and more research is underway.
If you are considering PRP for sexual health, the most important step is to find a provider who is honest, experienced, and equipped to assess and monitor your progress properly.
Nova Voya works with a network of verified clinics offering this treatment within structured, transparent care pathways, so you can explore your options with confidence and clarity.
Looking for a Verified Clinic for PRP Female Sexual Health Treatment? 🏥
Nova Voya connects women with thoroughly vetted clinics that specialize in PRP therapy for sexual dysfunction and pelvic health. Browse verified packages and get the support you need to make the right choice.
- ✔ Verified clinics with gynecology and pelvic health expertise
- ✔ Transparent treatment packages with no hidden costs
- ✔ Personalized guidance to help you find the right care pathway
*Verified Clinics Only
How do you feel about using your body’s own healing power, like PRP, to enhance sexual wellness and function; would you give it a try?
FAQs
It is an injection of platelet-rich plasma, made from your own blood, into the vaginal wall and clitoris to stimulate tissue healing, improve sensitivity, and restore sexual function.
The O-Shot is a trademarked name for vaginal and clitoral PRP injections used specifically for sexual enhancement and dysfunction treatment in women.
Studies show improvement in sexual desire, arousal, lubrication, orgasm, vaginal health, and emotional distress related to sexual dysfunction.
The standard clinical protocol is 3 monthly injections, one session per month for three consecutive months.
The most common dose used in studies is 2 mL injected into the distal anterior vaginal wall, sometimes with an additional injection into the clitoris.
The studies reviewed did not report pain as a significant side effect; mild discomfort from the needle is expected, as with any injection.
Fewer than 1% of women across all studies experienced side effects, and all were minor and resolved without treatment.
Studies tracked patients for up to 12 months; there is no published data yet on whether results are maintained beyond that period.
No, as of the 2023 systematic review it is not included in official clinical guidelines and is still considered investigational.
Yes, studies show significant improvement in stress urinary incontinence, though the dose and injection site differ from the sexual dysfunction protocol, and surgery still outperforms PRP in the only randomized trial available.


