If you had spine surgery and you are still dealing with pain, you are probably exhausted. Not just physically, but mentally. You trusted the process. You went through recovery. And yet here you are, months or maybe even years later, with pain that never really went away, or pain that came back stronger than before.
This is not a rare situation. Research published in the Journal of Yeungnam Medical Science found that between 5% and 27.6% of patients experience chronic pain after spinal surgery, with an average of around 15% across studies. That is roughly 1 in every 7 patients.
There is a name for what you are experiencing: Failed Back Surgery Syndrome (FBSS). And despite what the name might suggest, it does not mean the surgery was necessarily done wrong. It means your pain did not respond the way everyone hoped it would.
Understanding what FBSS actually is, what causes it, and what can genuinely help you move forward, is the first real step.
Scientific Source: This article is based on peer-reviewed research by Jinseok Yeo, “Failed Back Surgery Syndrome — Terminology, Etiology, Prevention, Evaluation, and Management: A Narrative Review,” published in Journal of Yeungnam Medical Science, 2024, Vol. 41, No. 3, pp. 166-178. DOI: https://doi.org/10.12701/jyms.2024.00339
Key Takeaways: (TL;DR)
- Persistent pain after spine surgery is more common than people think, affecting up to 1 in 7 patients
- This condition has a name: Failed Back Surgery Syndrome (FBSS), and it is not your fault
- The causes are varied: scar tissue build-up, wrong surgical level, adjacent bone degeneration, and more
- Not all treatments are equal: some work short-term, others offer lasting relief
- Revision surgery is usually not the first recommended step
- A proper evaluation is the most important thing you can do right now
- For patients in the UAE and Gulf region, Dr. Alireza Taghikhani offers specialized FBSS care at Al Zahra Hospital Dubai
What Exactly Is FBSS?
Failed Back Surgery Syndrome is a clinical condition defined by ongoing or recurring pain after one or more spinal surgeries, in the same area where surgery was intended to help.
According to the world’s leading authority on pain research, FBSS refers to lower back pain that either never fully resolved after spine surgery, or returned in the same region where the original problem existed, even though the procedure was intended to fix it.
In simple terms: the surgery happened, but the pain stayed or came back.
Some researchers now prefer calling it “Persistent Spinal Pain Syndrome” (PSPS) because the word “failed” unfairly places blame on either the patient or the surgeon.
The condition is complex, and pain after spine surgery has many possible causes that are not always predictable before the operation.
What is clear is this: FBSS is real, it is recognized medically, and there are structured ways to evaluate and treat it.
Why Does This Happen? The Real Reasons Pain Doesn’t Go Away
This is probably the question you have been asking since the surgery. The honest answer is that FBSS rarely has just one cause. Research identifies three broad categories of contributing factors.
It Started Before the Knife Even Touched You
Some factors that influence surgical outcomes are present before the operation ever begins.
- Psychological and emotional state plays a bigger role than most people expect. Studies show that depression, anxiety, and passive coping styles are among the strongest predictors of poor surgical outcomes, even more so than the physical structure of the spine itself.
- Social and workplace factors also matter. Patients going through workers’ compensation claims or active litigation tend to have less favorable results after spine surgery. This does not mean they are faking it. It means the environment around them, the stress, the legal pressure, affects how pain is perceived and reported.
- Lifestyle factors like smoking and obesity increase the risk of problems. Smoking specifically is linked to slower healing, higher infection rates, and a greater chance of needing reoperation. Excess weight is associated with less improvement in leg pain after surgery.
What Happened in the Operating Room
Surgery-related causes are often the ones patients focus on, and they are genuinely important.
- Wrong level decompression is a significant cause of FBSS. Performing surgery on the wrong spinal level, or only decompressing one level when multiple levels are involved, will not resolve the underlying problem.
- Incomplete decompression of the lateral recess or nerve openings is another common culprit. If the nerve is still being compressed after surgery, the pain will continue.
- Poor surgical technique can create new problems. Direct nerve damage, instability in a spinal segment, and reduced blood supply to the spinal cord during surgery can all introduce new sources of pain that did not exist before.
What Developed After the Operation
Even a well-performed surgery can lead to new problems over time.
- Scar tissue build-up inside the spinal canal, called epidural fibrosis, is one of the most common post-surgical complications. One study found that 83.3% of patients with FBSS had severe epidural fibrosis when examined directly. This scar tissue wraps around nerve roots, restricts movement, and creates both back and leg pain.
- Adjacent segment degeneration is another major issue. When one level of the spine is fused, the levels above and below it experience more stress. Over time, those neighboring joints, discs, and ligaments begin to break down. Research shows that 22% to 36% of patients develop this within 10 years, and more than 20% of those will eventually need additional surgery.
- Disc problems returning also happen. Among patients who had surgery for a herniated disc, the overall rate of reoperation was 15%, with 62% of those reoperations caused by the disc herniating again.
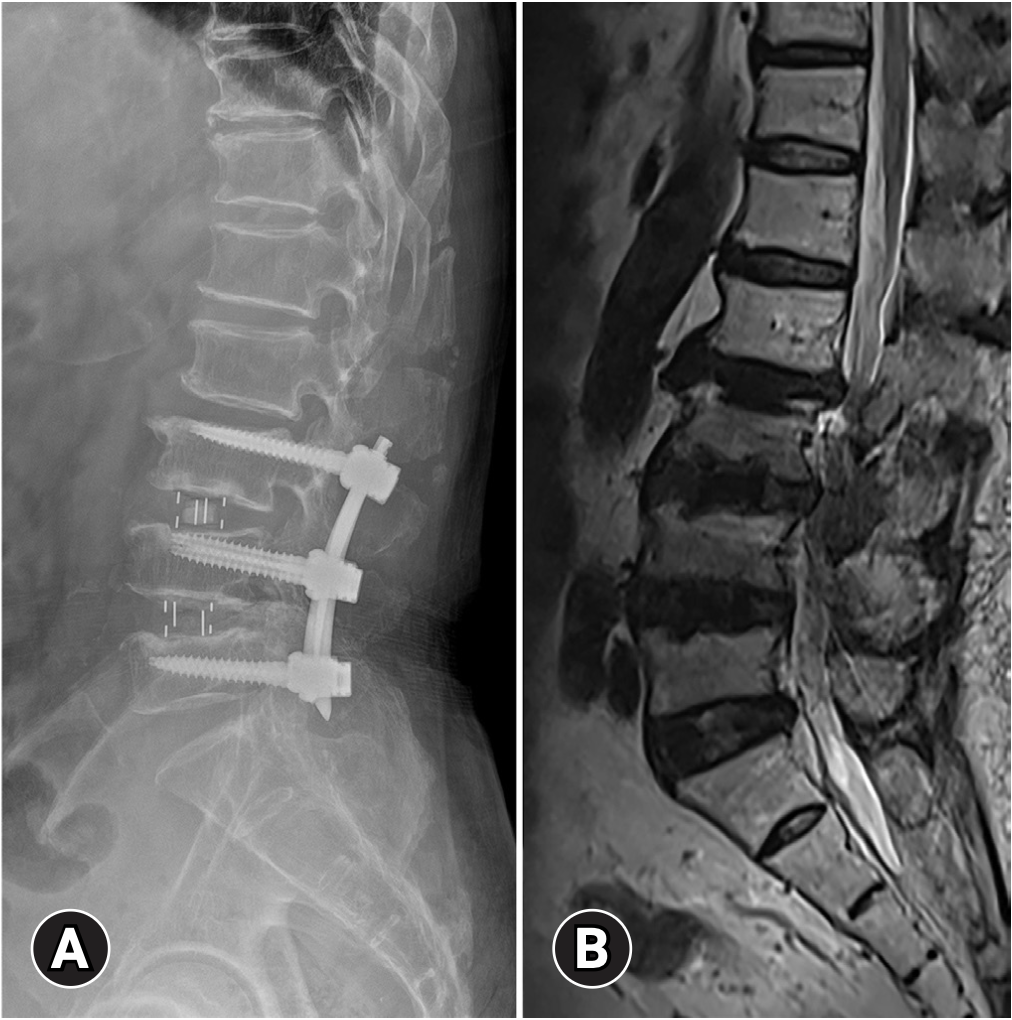
The Truth About Why Most Second Attempts Don’t Work Either
Here is something important to understand: many patients who are still in pain after surgery assume that another surgery will fix the problem. Research suggests this is rarely the right first move.
Revision spine surgery carries significantly higher risks than a first operation. These include a greater chance of new nerve damage, higher complication rates, and lower overall success rates.
The evidence is clear on this point: going back under the knife is not a reliable fix. Studies consistently show that reoperation delivers lasting results in only a small proportion of FBSS patients, which is why most specialists treat it as a last resort rather than a go-to solution.
This is not pessimism. It is a realistic picture that helps patients make better decisions and avoid unnecessary procedures.
Before considering any surgical revision, there are non-surgical and minimally invasive options that have shown real evidence of helping.
What Actually Works: A Look at Real FBSS Treatments
Treatment for FBSS works best when it involves a team approach, combining multiple types of care based on what is specifically causing your pain. Here is what the evidence says.
Targeted Injections to Quiet the Nerves
Epidural steroid injections can reduce inflammation around compressed nerves and offer meaningful short-term relief. Among the different injection approaches, the transforaminal method, which targets a specific spinal level, shows the strongest results for nerve-related pain.
For patients whose pain comes from the small joints at the back of the spine, called facet joints, a different approach is used. These joints are responsible for pain in roughly 16% of FBSS patients. Nerve blocks at these joints, followed by radiofrequency ablation if effective, can reduce pain for up to 12 months.
Scar Tissue Removal
Because epidural fibrosis is so common in FBSS, procedures that physically break up this scar tissue have become an important treatment option. Percutaneous adhesiolysis, which uses a small catheter to loosen adhesions, has significant evidence behind it.
A related technique using a tiny camera, called epiduroscopic adhesiolysis, has shown clinically meaningful pain reduction lasting 6 to 12 months in FBSS patients.
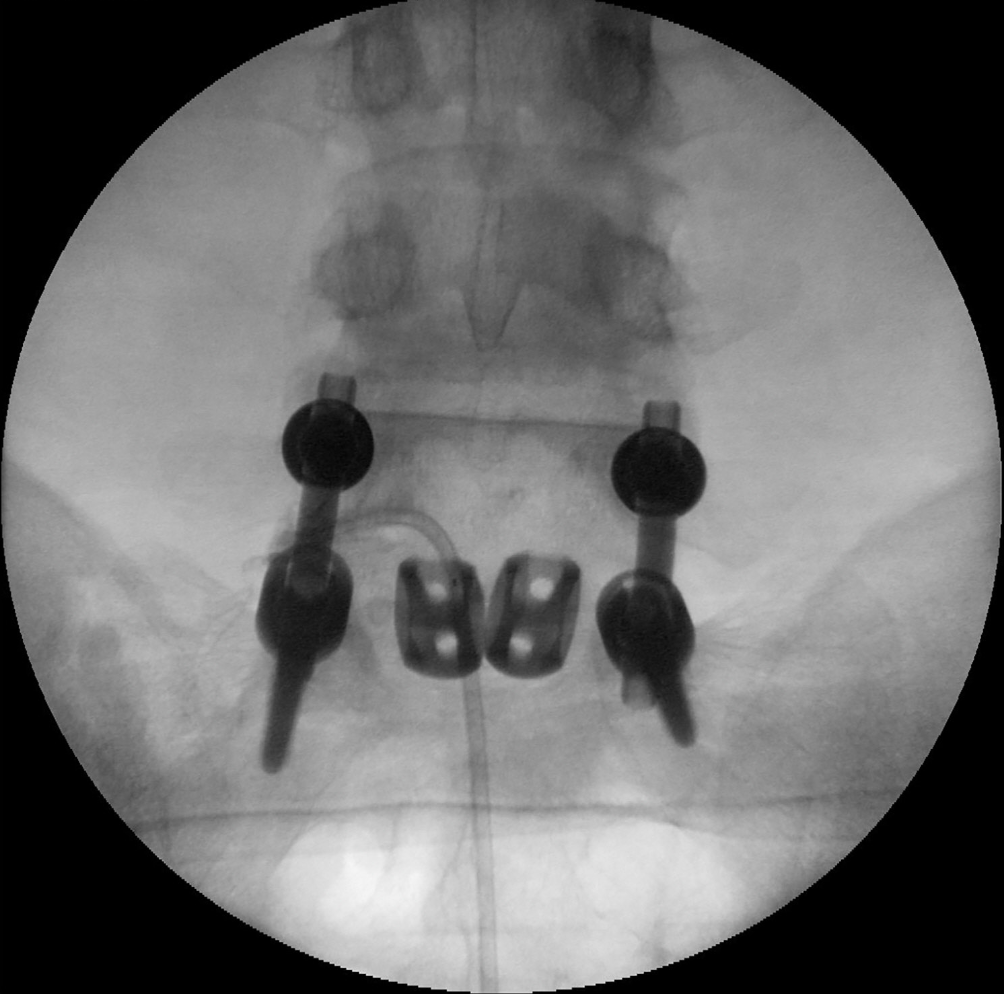
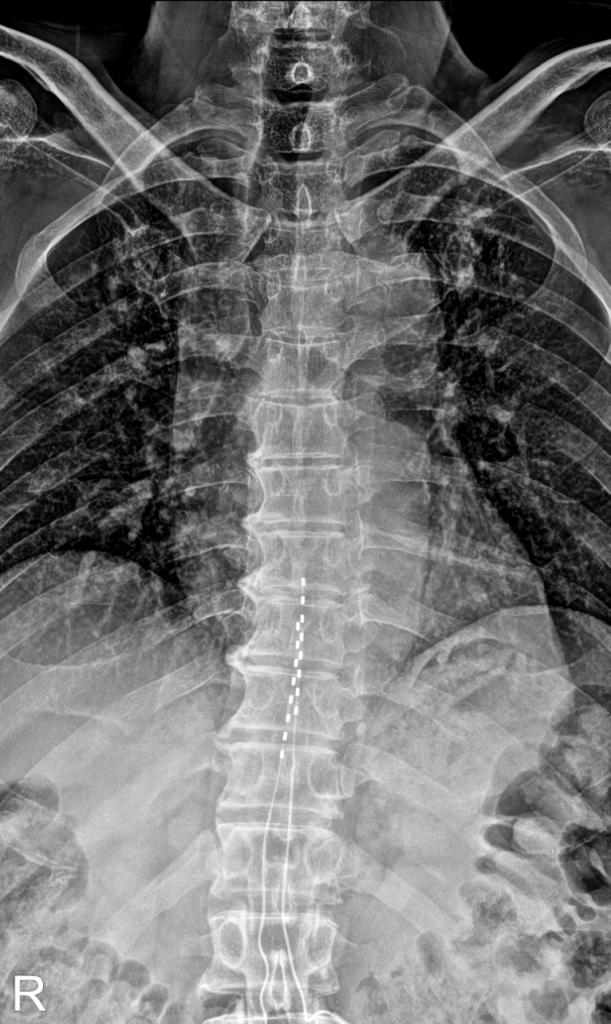
Spinal Cord Stimulation
For patients with persistent nerve pain that does not respond to other treatments, spinal cord stimulation (SCS) is considered one of the most effective options available. The device delivers gentle electrical impulses to the spinal cord, reducing the pain signals reaching the brain.
Multiple studies show SCS is more effective than reoperation for ongoing nerve-related or back pain after lumbar surgery.
It is also cost-effective when compared to repeated conventional treatments and offers something rare: a trial period before permanent implantation, so patients can test it before committing.
Physical Therapy and Exercise
Strengthening the muscles that support the spine is essential after surgery. FBSS patients often experience muscle weakening, particularly in the deep core and back muscles, which reduces spinal stability. Evidence supports structured exercise programs that include supervision, stretching, and progressive strength training.
The McKenzie method and Pilates are specifically highlighted in research as being more effective than general exercise for reducing pain and functional limitations.
Psychological Support
Because psychological factors so strongly influence outcomes, cognitive behavioral therapy (CBT) has solid evidence behind it for chronic pain management. It helps patients change how they think about and respond to pain, builds coping skills, and has been shown to reduce both pain and disability.
Is Revision Surgery Ever the Right Answer?
Yes, but only in specific situations.
Revision surgery is appropriate when imaging identifies a clear physical cause, such as a disc herniation returning, adjacent segment degeneration causing nerve compression, or a structural problem that cannot be addressed any other way.
The key word is “identified.” If the source of pain is not clearly visible on imaging, surgery is unlikely to help and carries significant risk of making things worse.
This is why a thorough evaluation, including detailed MRI or CT scans and a full clinical assessment, is the non-negotiable starting point for anyone with FBSS.
Who Should Actually Consider Specialized FBSS Treatment?
Not everyone with post-surgical back pain needs complex revision care. But some situations clearly call for specialist evaluation.
You are likely a good candidate for advanced FBSS treatment if:
- Your pain has persisted for more than 3 months after surgery with no sign of improvement
- You are experiencing new or worsening nerve symptoms such as leg pain, numbness, or weakness
- Previous treatments including physiotherapy and injections have not given lasting relief
- Imaging suggests a structural issue such as adjacent segment degeneration, recurrent disc herniation, or implant complications
- You have been told another surgery might be needed but want a second opinion first
If you are unsure whether your situation qualifies, a comprehensive evaluation is the only way to know.
Who Should Be Careful About Proceeding Too Quickly?
There are situations where slowing down is the wiser path. FBSS treatment requires careful planning when:
- There are significant unaddressed psychological factors such as severe depression or active litigation that may reduce treatment effectiveness
- Lifestyle factors like active smoking or uncontrolled obesity are present, as these reduce healing and surgical outcomes
- Imaging does not clearly identify the pain source, in which case surgical options are unlikely to help
- The patient’s expectations have not been realistically discussed with a specialist
Honesty about these factors leads to better outcomes. A good specialist will discuss them openly.
What to Expect: A Realistic Recovery Timeline
Recovery from FBSS treatment is not a straight line. Here is an honest picture of what the process looks like:
- First weeks: Initial relief from targeted injections or procedures, combined with physiotherapy to begin rebuilding muscle support.
- Weeks 4 to 8: Gradual improvement in function, reduced reliance on pain medications as other treatments take effect.
- 3 to 6 months: Meaningful recovery in mobility and daily activity, particularly for patients who engage consistently with physical rehabilitation.
- Ongoing: For some patients, SCS or long-term physiotherapy provides continued improvement over months and even years.
No treatment guarantees complete elimination of all pain. Realistic goals include meaningful reduction in pain intensity, better mobility, and improved ability to do daily activities.
Why Dubai for FBSS Treatment?
For patients across the UAE, Gulf region, and internationally, Dubai has become a trusted destination for complex spinal care.
Al Zahra Hospital Dubai holds JCI accreditation, one of the highest international standards for hospital safety and quality. The facility is equipped with advanced imaging systems and surgical navigation technology that allows for more precise procedures.
Meet Dr. Alireza Taghikhani
Dr. Alireza Taghikhani is a board-certified neurological and spine surgeon with more than 20 years of experience in neurosurgery and spine care across the UAE. Since 2000, his clinical focus has included surgical treatments for complex spinal conditions including cervical and lumbar disc problems, degenerative spine disease, and head and spine injuries.
He uses microscopic and minimally invasive techniques, including keyhole procedures, to reduce recovery time and minimize disruption to surrounding tissue. His expertise extends to pain management and functional neurosurgery, making him well-positioned to handle the complex, multi-cause nature of FBSS.
Dr. Taghikhani is a Fellow of the American Association of Neurological Surgeons and an active member of the Emirates Society of Neurological Surgeons. He also holds membership in the Congress of Neurological Surgeons and the Iranian Association of Surgeons.
He currently sees patients at Al Zahra Hospital Dubai as part of his specialized spine practice.
Myth vs. Reality: What Most Patients Get Wrong About FBSS
| Common Belief | What Research Actually Shows |
| “If surgery didn’t work, nothing will” | Multiple non-surgical treatments including SCS and adhesiolysis have strong evidence for FBSS relief |
| “A second surgery will fix what the first one missed” | Revision surgery has low success rates and higher complication risks. It is only recommended in specific, imaging-confirmed cases |
| “Painkillers are the main long-term treatment” | Long-term opioid use for chronic back pain has limited evidence and significant risks. Minimally invasive procedures often outperform medication |
| “FBSS means the surgeon made a mistake” | Many FBSS cases result from factors present before or after surgery, not surgical error |
| “Pain this long means permanent damage” | With the right multidisciplinary treatment, meaningful improvement is achievable even years after the initial surgery |
Summary
If you have been living in pain after spine surgery, the most important thing you can do right now is get a proper specialist evaluation. Not another round of the same medications. Not a premature decision about whether to have more surgery. A real assessment, backed by imaging and clinical judgment, that tells you exactly what is causing your pain and what options you actually have.
Nova Voya connects patients with trusted, specialist-led care like the FBSS program at Al Zahra Hospital Dubai. From coordinating your first consultation to supporting you through every step of evaluation and treatment, Nova Voya makes the path forward clearer and easier to navigate.
You have already been through enough. Let the next step actually count.
Get Specialist FBSS Care, Without Paying Full Price
Dr. Taghikhani’s FBSS package at Al Zahra Hospital Dubai. JCI-accredited. All-inclusive. Exclusively through Nova Voya.
- ✔ Full pre-op consultation, MRI/CT review & surgical plan included
- ✔ Up to 5 nights private hospital stay + physiotherapy, all covered
- ✔ Package price reduces cost: same surgeon, same hospital, no compromise
What has been the hardest part of your recovery after spine surgery: the pain itself, the uncertainty about what to do next, or feeling like no treatment has truly addressed the root cause?
FAQs
A consultation with a specialist like Dr. Taghikhani is the only reliable way to assess your specific situation. Nova Voya can help coordinate that first step.
FBSS is a condition where a patient continues to experience back or leg pain after one or more spinal surgeries intended to relieve that pain.
Research shows that between 5% and 27.6% of patients develop chronic pain after spinal surgery, with an average rate of around 15%.
Not necessarily. FBSS has many causes including pre-existing psychological and social factors, post-surgical scar tissue build-up, adjacent segment degeneration, and disease progression that are not always preventable.
Usually not as the first option. Revision surgery has low success rates and higher complication risks. Minimally invasive procedures and spinal cord stimulation often perform better and are recommended first.
Spinal cord stimulation (SCS) uses a small device to deliver electrical signals to the spinal cord to interrupt pain signals. Multiple clinical studies show it is more effective than reoperation for persistent nerve-related pain after lumbar surgery.
Diagnosis involves a detailed clinical history, physical examination, and imaging, typically MRI with contrast or CT scans, to identify the specific sources of ongoing pain.
Yes. Targeted injections, scar tissue removal procedures, spinal cord stimulation, physical therapy, and cognitive behavioral therapy are all evidence-based, non-surgical options for FBSS.